Simple Math: Demand+Brand Amplifies with Customer Experience
Healthcare

Simple Math is a four-part series introducing BVK’s demand+brand strategy for health plans. This fourth installment provides a deeper dive into the final demand+brand pillar: Customer Experience.
The world of health care has always been complex. With the advent of the pandemic, economic recession, and concerns about social justice, the complexities have grown exponentially. Consumers are struggling to make difficult decisions. Health plans are no exception, with consumers increasingly distrustful whether their needs will be met with affordable benefits with the providers they want.
Health plan marketers are tasked with growing and retaining member volume in the unique and complex environment. Being a sales-driven category with marketing often taking a back seat, the focus has inevitably been on features and benefits that are often indistinguishable from the next plan (and a far cry from features offered by national plans).
The formula for success involves some unique math: 1 + 1 = 3. No, this is not an addition mistake. Rather, it is a multiplication strategy. At BVK, we call it demand+brand. It is our strategy for telling a compelling and defensible story of business growth for health plans. Coupling values-based brand building with lead generation and customer experience best practices produces the potential for short-term sales and long-term growth and differentiation.
The upside of adding brand building (long-term growth/sustainability) to traditional health plan demand generation (short-term growth) is speed. While demand generation sometimes produces long-term sales growth, brand building + demand generation nearly always produces short-term sales growth that continues to build. Simply put: 1 + 1 = 3.
Customer Experience
The final pillar of the demand+brand strategy is the customer experience during acquisition as well as after they become a member. Customer experience is foundationally about the individual and their desire for meaningful connection to fulfill a need. With four constructs of connection—full continuum, personalized touchpoints, personalized products, and provider integration—we will focus the marketing driven aspects where trust can be either earned or lost.
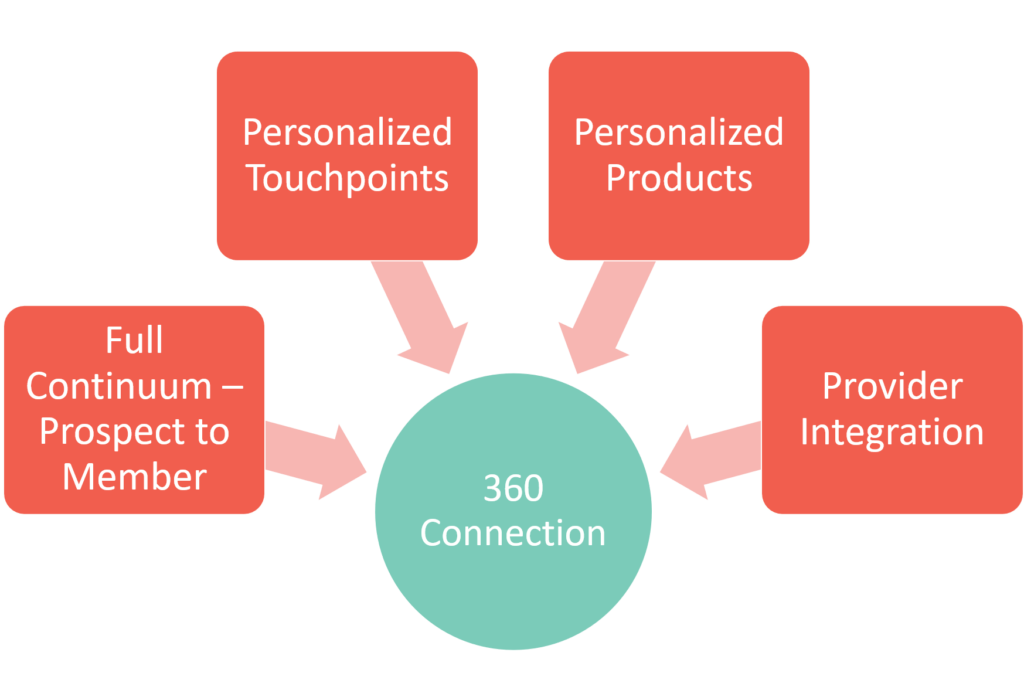
Full Continuum
The full continuum from prospect acquisition through member engagement, loyalty, and eventual advocacy is encompassed within the scope of customer experience. Most health insurance companies focus solely on net new sales and the importance of member experience is often overlooked. Because of this, retention, and brand building through word of mouth tend to be underdeveloped. By spotlighting moments of truth that are crucial to health plan members, experience enhancement can create long-lasting impressions.
Moments of Truth
- Researching
- Quoting
- Enrollment
- Onboarding
- Customer Service
- Billing
- Issue Resolution
Member retention is more than a flawless onboarding or exemplary customer service. We believe it must be part of the fabric of a company: an organizational imperative with an accountable cross-functional team. This team should use data-based, insight-driven decision making that integrates member personas and customized messaging that meets each audience’s specific needs. This type of demographic, behavioral, and attitudinal data can inform communication strategies and tactics. A retention team must always have a ‘test and learn’ posture to best optimize what works and find new approaches to engage members. Finally, there should be a concerted effort to listen and empathize with members. Customer service must understand exactly which touchpoints members have experienced so they can tailor an appropriate response.
Personalized Touchpoints
Personalization is no longer a luxury or a distinction for brands, it is expected and demanded by consumers, including in healthcare. Health plans have the opportunity to personalize app and website experiences based on consumers’ last interactions. Text and voice strategies also promote an individualized experience. Of course, your lead generation personalization through precision targeting and preferences is an imperative. No matter where you start nor how far along you are in the process, taking that first step toward an intimate consumer experience is vital to acquisition, loyalty and advocacy.
Personalized Products
The fracture event of the pandemic has changed the face of literally everything we do including how consumers interact with their health plans. A strong virtual care platform and corresponding coverage is essential for managing illness and wellness during this time and going forward. Additionally, insurance products and plans that focus on key disease states like diabetes, asthma, heart conditions and cancer offer help managing the costs of chronic conditions while also offering customer service benefits of pre-packaged medication and custom care journeys. Marketing no longer lives in the world of awareness and acquisition alone, rather a 360-degree customer experience that necessitates partnering with product development and marketing teams.
Provider Integration
An important last marker of customer experience is seamless integration with Providers. One of the top health insurance customer friction points is a tug-of-war between their care and access. Developing an integrated communication flow, scheduling, wellness care and billing satisfies consumer expectations and eases the burden of receiving healthcare today.
Best Practices
- Build a Customer Engagement and Retention Plan: Data-driven member experience strategy, tactics, and pilots
- Create Organizational Integration Centered on the Customer: Product, Operations, Sales and Marketing integration as well as Providers
- Employ Personalized Connection Planning: Full journey planning focused on personalization
We welcome the opportunity to talk with you further to discuss the simple math of our demand+brand strategy and how it can add up to plan growth for your organization. Feel free to reach out to [email protected] with questions or comments.
