The ‘Shot Clock’ in Health Care: Margin Challenge as a Function to Force Change
Healthcare

In basketball, the shot clock serves as a forcing function to keep the pace of play moving. It allows teams enough time to set up their play, while preventing the pace of the game from stalling out as players wait for an open shot.
In health care, there is no shot clock. Historically, there has been no real penalty for being slow to make and execute on the strategies needed to improve performance. This has been especially true for productivity and cost efficiency. Growing demand usually created enough new revenue to offset flat productivity and rising organizational costs. Even in cycles when utilization did slow, episodic cost-cutting campaigns were enough to maintain operating margins until demand recovered.
That dynamic has changed, and likely forever.
Recent trends of slowing utilization look less cyclical and more structural as high-deductible plans change consumer behaviors. Rising labor costs and pharma utilization, coupled with increasing cost of supplies and purchased services are outpacing gains in productivity and reimbursement. As a result, the gap between revenue and expense is greater now than even during the most challenging years of the Great Recession (Source: Moody’s Investor Service).
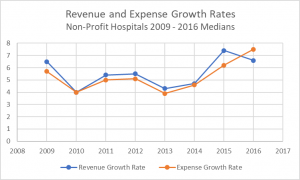
Starting from the 2015-2016 average hospital operating revenue and expense growth rates of 6.6% and 7.5%, respectively, and trending those rates back to post-ACA averages through 2025, it is likely that in the coming years many providers will see unsustainable negative margins, unrealized incentive payments and being shut-out of premium contracts for failure to perform to rising expectations.
At a macro level, the margin challenge is likely to create further shakeout in the health care industry. Congressional Budget Office (CBO) estimates, for example, show that unless providers increase productivity or reduce cost growth in some other way, it is possible that 60% of hospitals will have negative profit margins by 2025 and the average profit margin will fall to negative 0.2 percent. Let that sink in for a moment.
The path forward starts with leadership
Launching another cyclical, cost-cutting campaign is not enough to resolve the gap between revenue and expense growth rates. Structural change is needed. Governing boards and executive teams must directly confront the challenging questions about the value of being a system or network, and how they might restructure to deliver greater value at radically lower cost.
Frequently, identifying how to restructure is not the greatest challenge facing systems. It is acting on the critical strategy decisions and mobilizing people to execute them. System and network leaders often avoid conflict, re-litigate strategy decisions and short-arm accountability for change. Frequently, they simply “pave the cow paths,” applying new technology to old, inefficient processes without making the difficult decisions needed to radically improve productivity or change cost trends.
Even when confronted with a potentially existential threat like the growing gap between revenue and expense growth rates, health system leaders frequently struggle to see their situation differently. As the famous economist John Kenneth Galbraith once observed, “faced with the choice between changing one’s mind and proving that there is no need to do so, almost everybody gets busy on the proof.”
Brand+Lever believes that change starts in the minds and will of the leaders to stop doing what no longer works and to build a vision and mobilize people to execute strategies to create new value. To learn more about our approach, contact Mike Eaton at (757) 784-1277 or [email protected]. Be sure to do so before the shot clock runs out!